You are here: Home > Our Services > Specialised Procedures > Fibroids
Uterine Artery Embolisation for the treatment of Fibroids
Fibroids are the single most common cause of hysterectomy, accounting for one third of the 70,000 performed by the NHS on women in the UK every year.
There are several alternatives to the treatment of fibroids by hysterectomy. These are myomectomy, hormone treatment and uterine artery embolisation.
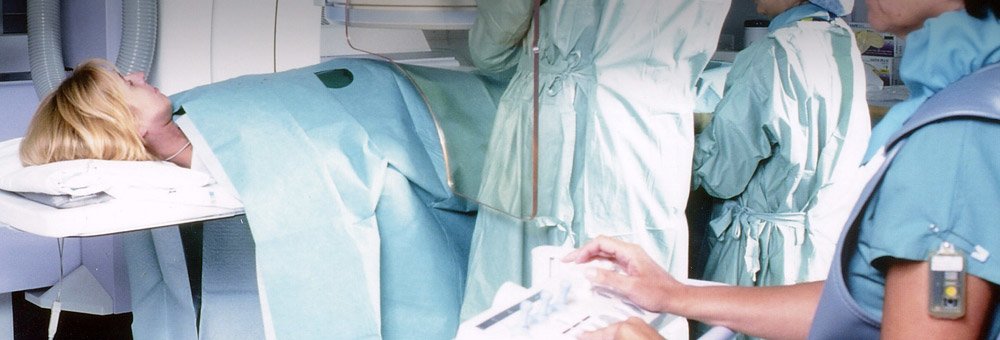
Uterine artery embolisation is a process by which fibroids are starved of their blood supply by blocking the supplying arteries with small particles. The procedure can be carried out in the new interventional suite in St Anthony's and is performed by a specialised vascular interventional radiologist. Some sedation is given and the procedure is performed under local anaesthetic. A plastic tube (catheter) is inserted into the two arteries which supply the uterus. The catheter is guided to these arteries by the radiologist and a special X-ray dye is injected to identify the blood vessels. Once the radiologist has located the blood supply, he or she can inject fluids containing thousands of tiny particles into the artery and these particles silt up the small blood vessels and block them, so starving the fibroid of its blood supply. Hospital stay is usually one to two days and the patient is advised to take at least two weeks off work.
A Joint Working Report published in January 2001 by the Royal College of Radiologists and the Royal College of Obstetricians & Gynaecologists concluded that uterine artery embolisation (UAE) should be considered for women with symptomatic fibroids who might otherwise be advised surgical treatment. It is recommended that women with symptomatic fibroids should be seen, in the first instance, by a gynaecologist. If it is deemed appropriate, the embolisation procedure should then be undertaken by a radiologist with specialised embolisation experience. Many thousands of uterine artery embolisation procedures to treat fibroids have been undertaken since 1991. Although long term results are still not available, around 80 – 90% of women are happy with the result. Measurements with various scanning techniques have shown an average reduction of around 50% in the size of the fibroid uterus, although this may take several months to occur.
Complications may occur but are rare. One of the most significant complications is of severe infection which can occur up to three months following the procedure. Severe infection has been associated with one death following the procedure, and in cases of severe infection a hysterectomy may be necessary. Different instances of this complication have been noted, with up to a 2% incidence of infection requiring hysterectomy. Lesser degrees of infection are treated with antibiotics, and sometimes minor gynaecological procedures are also necessary. The other main complication is that menopausal changes have been noted following the procedure. This seems to occur in women who are at or close to the menopause, but the true incidence of this early menopause is around 1%. Better and longer term data are necessary, but it is believed that once the fibroids have shrunk they do not grow back, and it also appears that new fibroids do not form.
The effect of embolisation on fertility in women who might want to become pregnant sometime in the future is still not known and there are no good available data, but a number of successful pregnancies following embolisation for fibroids and other conditions have occurred, with a normal successful outcome.
NOTE: This information has been taken from clinical recommendations on the use of uterine artery embolisation in the management of fibroids: Report of a Joint Working Party, Royal College of Radiologists and the Royal College of Obstetricians and Gynaecologists.
For further information send us a message on the feedback page or telephone the Help Desk on 020 8335 4646.
FEmISA web site
(Fibroid Embolisation Information, Support and Advice)
www.nice.org.uk/pdf/ip/IPG094publicinfo.pdf
(The National Institute for Clinical Excellence, Uterine artery embolisationfor the treatment of fibroids PDF)
www.fibroidnetworkonline.com
(Fibroid Network Charity Online World Fibroids Information website)


 Click here to get help
Click here to get help