You are here: Home > Our Services > Specialised Procedures > Early repair of cartilage injuries of the knee
Early repair of cartilage injuries of the knee
Articular cartilage is the slippery surface lining all moving joints in the body. It is unique in being formed of a type II collagen meshwork with proteoglycans produced by the cartilage cells. Unfortunately, when damaged by injury or arthritis it is not capable of repairing itself except sometimes with scar tissue which breaks down easily leaving bare bone exposed. Hunter in 1746 stated “articular cartilage once depleted does not recover” this remained true for the next 200 years.
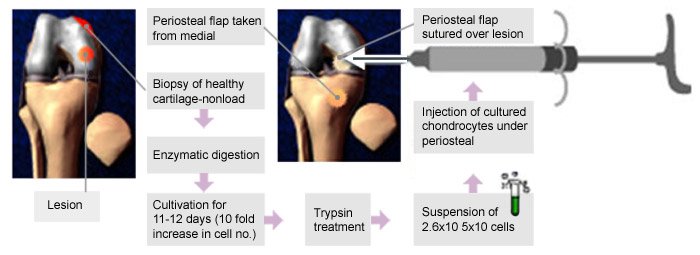
ACI technique
As a consequence young people who have injuries to joints or develop conditions such as osteochondritis or avascular necrosis which cause damage to cartilage can often receive no useful treatment for their painful disability. Also, these conditions progress to early osteoarthritis in patients who are too young to undergo joint replacement. This is a particular problem in the knee joint and it is conservatively estimated that 10,000 people per year, in the UK, suffer from such injuries and receive inadequate treatment at present which reduces their activities and pre-disposes them to early osteoarthritis. Over the last two decades new advances in cell therapy has started to change this state of affairs. The initial attempt to stimulate the marrow cells resulted in fibrocartilage (scar tissue) which rapidly broke down. The current techniques which involve transplanting cartilage allograft (tissue taken from human donors) or the culturing of cells in modern laboratories under stringent conditions and then transplanting into the knee have provided hope to this group of patients.
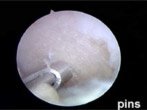
Preparation of cartilage defect with microfracturing and then pinning of the collagen scaffold
Cartilage transplant is now available at St Anthony's Hospital.
Mr Adhikari, one of our Consultant Orthopaedic Surgeons with a special interest in knees, has been involved in cartilage research for the last 8 years. He uses two techniques at present one of which is also part of a multicentre pan-European trial. Membrane Articular Cartilage Implantation entails the harvesting of cartilage cells from the patient arthroscopically. These are then sent to a laboratory in Denmark where they are cultured to produce around 5 million cells over a period of 4 to 6 weeks. The cells are impregnated into an artificial collagen membrane which acts as a scaffold for cartilage production. This membrane is then transplanted into the cartilage defect in the knee. Subsequent physiotherapy rehabilitation is tailored to help the cartilage to provide a strong and durable surface.
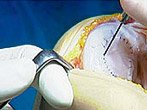
Membrane over cartilage defect
The second technique involves the stimulation of bone marrow cells at the base of the cartilage defect by microfracture and then these cells are contained within the defect by fixing a collagen membrane with fibrin glue and dissolvable micropins. Physiotherapy is again important postoperatively
These techniques are still only suitable for those patients who haven’t already progressed to osteoarthritis and studies show success rates of up to 80 percent depending on the site of the cartilage defect.


 Click here to get help
Click here to get help